The Candida auris fungus is once again setting off alarms in hospitals across New York and New Jersey due to its drug resistance and the speed at which it can worsen the situation
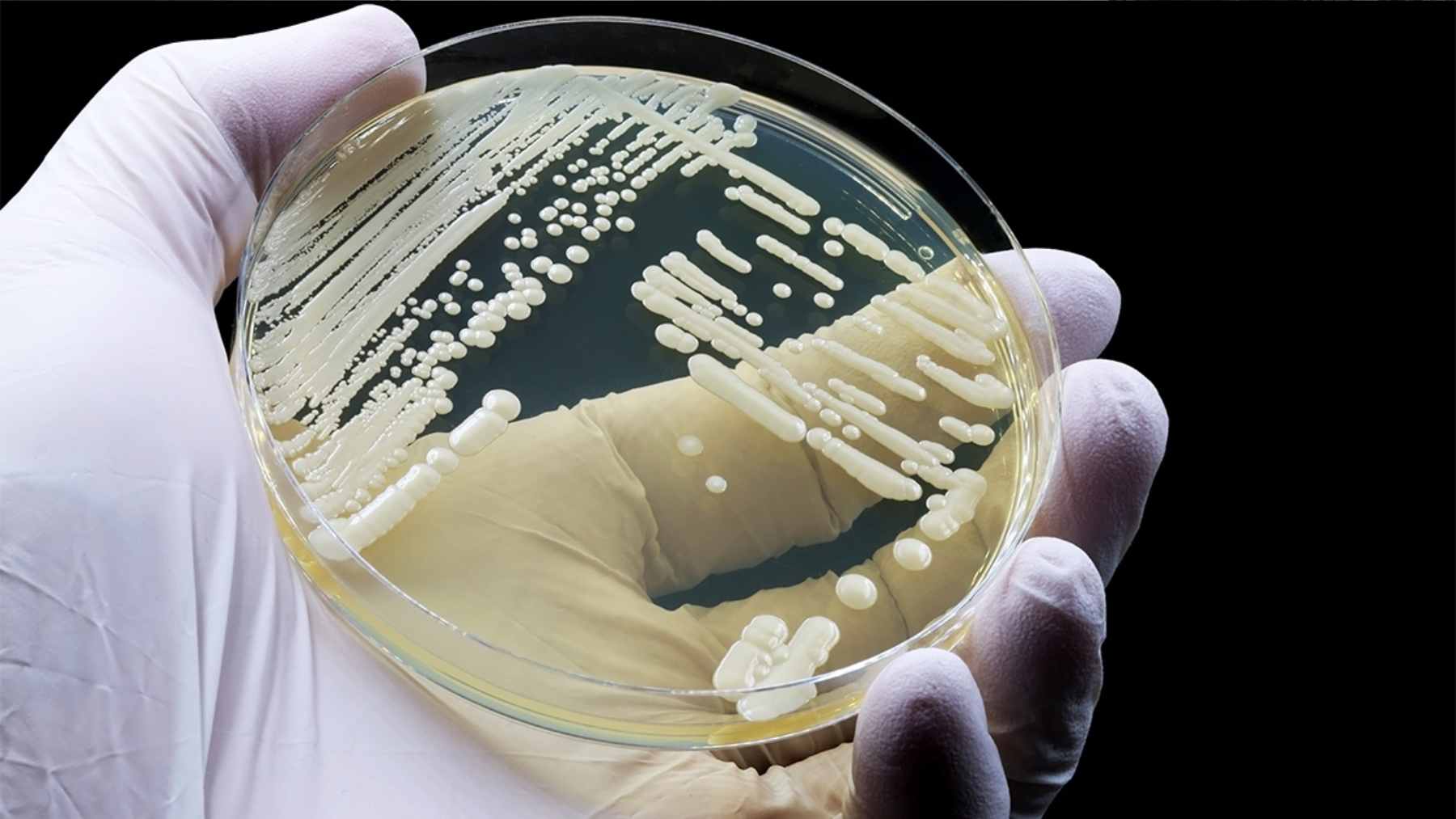
Hospitals across the New York and New Jersey region are tightening routines around an unusually stubborn fungus called Candida auris. In 2024, the Centers for Disease Control and Prevention recorded 6,304 clinical cases in the United States, a sign that this germ has become a steady, nationwide challenge inside health-care facilities.
What makes this story different is how the fungus spreads and why the New York and New Jersey metro area keeps showing up in the data. A study led by Vishnu Chaturvedi at New York Medical College points to a mix of international travel and local patient movement between facilities, which can quietly carry the fungus from one ward to another.
A yeast that behaves like a superbug
Candida auris is a yeast, a type of fungus, but it acts more like a “superbug” than a typical yeast infection. It can cause severe illness when it gets into the blood or other parts of the body, especially in people who are already very sick.
Part of the challenge is that Candida auris can live on skin without causing symptoms, a state doctors call colonization. That makes it easier to spread without being noticed, a bit like tracking glitter after a craft project – you do not see it until it is everywhere.
Why New York and New Jersey stand out
Local health departments have found that the regional footprint is unusually large. The New Jersey Department of Health reported 3,402 total detections as of February 1, 2026, including 754 clinical cases and 2,648 screening cases, which are people carrying the fungus without signs of illness.
New York City’s role as an international travel hub may be part of the story, but it is not the only factor. Extended-stay care facilities and frequent patient transfers can create a chain that links many buildings, even when no single hospital thinks it has an outbreak.
Why it is tough to control inside health care
Candida auris is hard to kill on surfaces, and it can linger on bedrails, monitors, and shared equipment if cleaning slips even a little. That staying power matters because hospitals are busy places, and the smallest shortcut can snowball into a bigger problem.
The fungus also has a talent for hanging around in the places where the sickest patients spend the most time. Think intensive care patients with catheters, ventilators, or weakened immune systems – once Candida auris gets in, it can be serious.

When medicine falls behind
Treating Candida auris is not as simple as reaching for the usual first-choice drug. A CDC analysis published in the Emerging Infectious Diseases journal found that 95% of tested isolates were resistant to fluconazole, and 15% were resistant to amphotericin B, two major antifungal options.
This is also part of a bigger pattern that goes beyond fungi. The World Health Organization has warned that antibiotic resistance is rising fast, and it can turn common infections into much harder problems to treat.
How antibiotic misuse feeds resistance
Doctors have been warning for years that unnecessary antibiotics can do real damage, both to patients and to the wider health system.
Aaron Glatt, who leads the Department of Medicine at Mount Sinai South Nassau, has said antibiotics should not be used for viral illnesses like colds and flu, because that only gives microbes more chances to adapt.
That pressure can help select for stronger and stronger defenses, especially in bacteria. It is one reason researchers keep tracking antibiotic resistance and the spread of hard-to-treat germs in hospitals, where the most vulnerable patients often have the least room for error.
What hospitals are changing right now
The first line of defense is finding it early, even before symptoms show up. Screening often uses a simple skin swab, typically taken from areas like the armpit and groin, to catch colonization before it turns into a wider outbreak.
Facilities also focus on isolation, careful use of gowns and gloves, and more aggressive cleaning with products proven to work against this specific fungus. Many rely on the Environmental Protection Agency list of disinfectants expected to be effective against Candida auris when used correctly.
A policy push to speed up new antibiotics
Even when scientists find promising drugs, the economics can be messy. Antibiotics and antifungals are often held in reserve, so companies may not earn enough to justify the massive cost of research and development.
That is why Congress has revisited the PASTEUR Act, which proposes a subscription-style model where the government would pay for access to critical new antimicrobials, even if doctors try to use them sparingly.
Ultimately, it is an attempt to keep the pipeline moving before the next super strain makes today’s treatments obsolete.
What this means for patients and families
For most people in the community, the risk remains low. But for patients in hospitals and long-term care facilities, especially those with complex conditions, Candida auris is one more thing clinicians have to stay ahead of, alongside other drug-resistant bacteria.
If you have a loved one in long-term care, it is reasonable to ask about infection control practices, not in a confrontational way, but as a basic safety question. Small steps, like clean hands and clear transfer paperwork, can matter a lot when the enemy is invisible.
The main study has been published in Microbiology Spectrum.
What's Your Reaction?
 Like
0
Like
0
 Dislike
0
Dislike
0
 Love
0
Love
0
 Funny
0
Funny
0
 Angry
0
Angry
0
 Sad
0
Sad
0
 Wow
0
Wow
0














































